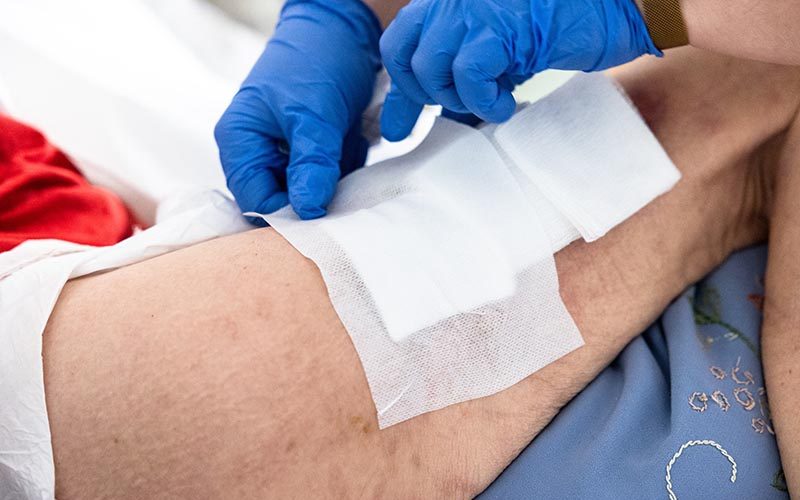
Bed sores, or pressure ulcers, are a constant threat to nursing homes. According to a study by the Centre for Disease Control and Prevention (CDC), one in ten nursing home residents develops pressure ulcers. This statistic is alarming, but it gets worse.
The likelihood of developing pressure sores increases if the senior has severe mobility problems, like being bedridden or using a wheelchair. For elders— the demographic with the highest probability of suffering from these mobility issues —these odds are unfavourable.
Pressure ulcer prevention is crucial because the costs of treating this pressure induced injury aren’t cheap. Depending on the severity of the sores, the hospital bills may get as high as $40,000. That is seen in the case of the patient in this study.
It would be best to know all about the causes of bedsores so as not to expend valuable resources on treatments. This is crucial if you have an elderly loved one in a nursing home.
What Are Bedsores?
Bed sores, or decubitus ulcers, are injuries that occur on the skin when a person stays in one position for prolonged periods. These pressure sores form when the body’s weight cuts off blood supply to the skin of that area, killing it. Bony parts of the body are notorious for developing pressure ulcers. These include the tailbone, the shoulder blades, and the heels.
In the early stages, they start as small reddened areas on the skin that are easy to deal with. But if the skin is under pressure for longer, it may extend to the bones and muscles. At this point, the bed sores can cause life threatening infections and several other health conditions that may even be fatal.
It is easy to develop pressure ulcers, yet it’s costly to treat, so nursing home staff usually take stringent measures for pressure ulcer prevention.
Bed sores are graded into four levels based on their severity.
- Stage 1 Pressure Ulcers: These are early-stage bedsores and the mildest of them all. Here, only the upper layer of the skin is affected by the prolonged pressure. There will be some pain and discolored skin which won’t get lighter when pressed due to the lack of blood supply. This may be difficult to notice on people with dark skin.
- Stage 2 Pressure Ulcers: When the sores get past the skin’s first layer, it leaves an open wound or a blister on the affected area. The area will be swollen, red and painful.
- Stage 3 Pressure Ulcers: These exhibit full thickness skin loss, where all layers of the skin and the surrounding tissue have been compromised. The sore would look like a crater with pus.
- Stage 4 Pressure Ulcers: Three are the most life-threatening. At this point, the sore has eaten its way to the muscles and bones, causing extensive skin damage. Due to the dead tissue surrounding the crater, here is a high risk of fatal infections and complications here.
What Causes Bedsores In Nursing Homes?
Many factors work hand in hand to bring these sores about. While sustained pressure on the same position is the prime culprit, there are other causes of bedsores that are important to note. There are also some risk factors that increase the likelihood of developing pressure ulcers. We’ll take a few of them here.
- Lack Of Mobility: Pressure on the skin can be easily alleviated by movement. That becomes difficult when the senior has impaired mobility. When there is no one to help them change position, there will be prolonged pressure, and these sores will form.
This is one of the most notable causes of bedsores.
- Incontinence: Fluids on the skin surface increase the occurrence of these pressure sores. This is where adequate hygiene comes into play. If incontinent people aren’t cleaned properly, they are more likely to develop these injuries. That is one of the leading causes of bedsore.
- Poor Nutrition: A lack of some essential nutrients can cause weight loss, predisposing seniors to pressure ulcers. Poor nutrition is also one of the causes of skin breakdown, which leads to pressure sores.
- Diabetes: Diabetic people have lower blood flow in their blood vessels, giving them an increased risk of developing pressure sores.
- A Low Or High Body Mass Index: The body’s fat is a telling factor in the emergence of bedsores. If it is too little, there won’t be enough padding for the bones. On the other hand, the excessive weight of a person with a high BMI would increase the pressure on the skin, leading to pressure injuries.
- Poor Hygiene: When a patient isn’t cleaned properly, pressure ulcers can occur. This is more important if they are incontinent or suffering from diabetes. Having fluids on their body can increase the probability of these injuries occurring.
- Age: Older people have less elastic and fragile skin susceptible to pressure sores. They are also more likely to be victims of the other causes of bedsores.
Prevention Of Pressure Ulcers
Due to the high cost of treatment, it would be best to know the methods of preventing pressure ulcers. Armed with this information, you can prevent your loved ones the pain, discomfort, and loss of funds that these injuries would cause.
- Proper Nutrition And Hydration: Pressure is not the only factor that causes these injuries. A lower blood circulation can make a patient more susceptible to this injuries. A balanced diet brings about a constant flow of blood and healthy skin.
- Good Hygiene: The skin should be kept dry and clean to prevent pressure injuries, as fluids can increase the risk of their development. Adequate cleaning at the appropriate times would prevent pressure sores.
- Frequent Repositioning: The sores only come if the patient stays in one position for too long. This act of moving them around prevents that, and helps to relieve pressure. Healthcare professionals would have to help an individual with a spinal cord injury to move themselves.
- Quitting Smoking: Smoking is notorious for lowering the blood circulation. This gives a higher risk of developing bed sores. For that reason, preventing a bedridden or wheelchair-using patient from smoking is a good idea.
- Special Beddings: Cold skin has reduced blood flow to the extremities, so try keeping your loved one covered with special beddings. Some of them are made with bedridden patients in mind. These include special articles like air or water mattresses that relieve pressure, and special foam pads.
Some beds even have an automatic turning feature to prevent pressure sores. However, this may not be the best way to change position, as it might leave some parts of the body under constant pressure. It would be best if you use that feature while still repositioning your loved one manually.
Complications That Arise From Pressure Ulcers
If pressure ulcers are left to grow unchecked, they can lead to some life threatening complications. In a scenario where the elder suffering from the bed sores receives the best care and attention, you won’t have much to worry about.
However, if they have severe mobility issues, like spinal cord injuries, and are being neglected, their injuries are at risk of developing into more serious issues. This risk assessment is higher when the pressure sore is at the later stages.
- Cancer: Squamous cell carcinoma is a skin cancer that occurs when an area of the skin is a victim of constant pressure sores. This condition doesn’t look serious at first, but it could spread to the lymph nodes, and other organs. This spread could lead to death if left untreated.
- Bone And Joint Infections: If the pressure ulcers are at a later stage, especially stage 4, then good hygiene is paramount. At stage 4, the pressure sore has eaten through the skin and underlying tissue, leaving the bones and muscles open to the surroundings.
When the deep wound isn’t kept clean, bone and joint infections can occur. Infections like osteomyelitis and septic arthritis can set, severely hampering the movement of the already mobility impaired individual.
- Cellulitis: The skin and connective tissue in that area are susceptible to infection because of the harm the pressure sore has caused. Cellulitis is inflammation of the skin by bacterial infection.
Numerous indications of infection, such as warmth, edema, and inflammation, are brought on by cellulitis. Cellulitis is accompanied by pain, however those with neuropathy may not experience it due to the nerve damage.
- Sepsis: This is another complication that is caused by poor hygiene and subsequent infection of the pressure injury. When the body is infected, it will have to fight back. However, there are some times when the body’s retaliation might damage its own cells. This is called sepsis.
If the germs are too numerous, the patient may go into septic shock. This is a critical state where there is a marked reduction in the blood pressure. The blood won’t be able to get to all the organs that need it, which could lead to multiple organ failures and death
- Abscesses: These are painful bumps that occur on the skin. They are usually larger than pimples, and situated in the deeper layers of the skin. They are filled with pus, which collects as a result of infection. In this case, the infection is caused by the pressure sore.
These seem relatively harmless, but when left untreated, they can lead to their own complications. These include tissue death, endocarditis (an infection of the heart’s inner layer), and sepsis.
Treatment Of Bedsores
In the event of these bedsores, there are a few methods of medical care that can be taken for treatment. If you notice the early signs of bed sores, then treatment would not be too difficult.
- Treatment and Wound Care: Most complications from pressure ulcers are caused by infection, so preventing it should be a top concern. Healthcare providers should keep the skin clean and dry while treating pressure sores.
One of the skin care methods is keeping it dry by dusting cornstarch around the area, after cleaning with mild soap. However, you should be careful. Cornstarch on open sores is not advisable as bacteria can feed on it and multiply in the wound, causing more harm.
For the open wound, cleaning with saline solution each time the dressing is changed is a good idea.
Additionally, negative pressure wound therapy is an option. This is where a device sucks out the pus from the wound to aid the healing process. The dead skin can also be debrided for better recovery of the healthy tissue.
- Pressure Removal: Relieving pressure is essential in treating pressure sores to prevent the condition from worsening. Rearranging the bedding and adding extra pads accomplishes this. To keep the blood circulating, the person would also need to move once every two hours.
- Prescription Of Antibiotics And Better Diet: Antibiotics are typically used to fight infection when the pressure sore is at stage three or above.
Enough hydration and other nutrients will aid the wound healing process by reversing tissue damage and boosting blood flow.
- Surgical Methods: Bed sore treatment might require the use of surgical instruments. Procedures like dead tissue debridement to help the sores heal would cost a lot, so preventing pressure ulcers should be a priority.
Are Bedsores A Sign Of Neglect?
Healthcare professionals know about the prevalence of bedsores in nursing homes and should take steps to prevent them. So, the answer would be yes. Most of the time, the pressure ulcers nursing homes encounter result from negligence.
The good thing is that you can get compensation for the damages to your loved one when you collaborate with a qualified nursing home abuse law firm to take legal steps.
At Just point, you can get a free legal case review, then sit back as we match you with the best attorney for your case in seconds. Our lawyers and health professionals are ready to analyze your case and ensure you get all the compensation you deserve.
We are here to answer whatever questions you may have, be they medical or legal. Let us ensure that you are informed as you make your decisions.