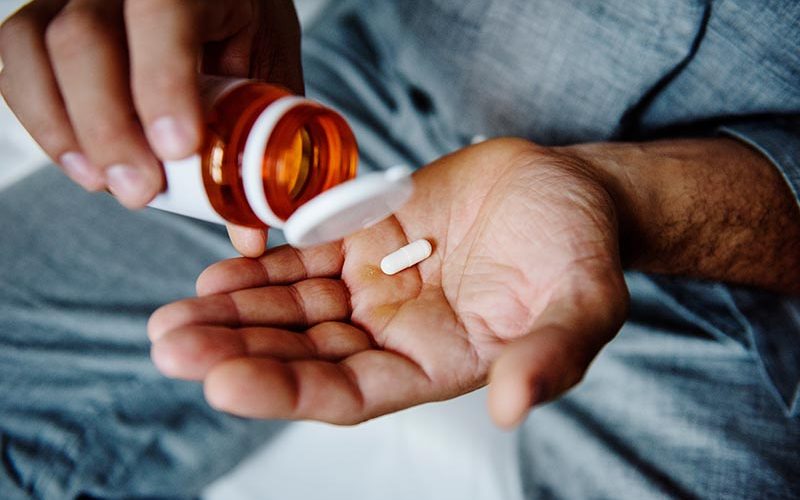
According to the National Coordinating Council for Medication Error Reporting and Prevention, a medication error is “any preventable event that may cause or lead to inappropriate medication use or patient harm while the medication is in the control of the healthcare professional, patient, or consumer.”
In other words, a medication error occurs when a doctor, nurse, or pharmacist does not properly prescribe, distribute, or regulate medication, which then causes – or has the potential to cause – harm to the patient.
Medication errors that cause harm are also known as preventable adverse drug events. A medication error that doesn’t harm the patient is called a potential adverse drug event, and would be prohibitive in bringing a lawsuit because of lack of injury.
When medication and drugs are prescribed and distributed, your healthcare provider has a duty to make sure that you receive the correct drug and the proper dosage of that drug.
Every year, over 1.5 million people are affected by medication errors in the United States. If you’ve been injured as a result of a medication error and your healthcare provider’s negligence, you may be a victim of medical malpractice and entitled to monetary compensation related to the medication error.
Types of Medication Errors
There are various types of medication errors that can occur as a result of your healthcare provider’s negligence.
According to an FDA study, the most common medication error is the prescription of the incorrect dosage, which makes up 41% of fatal medication errors.
Prescribing the wrong medication and providing incorrect drug instructions (i.e. improper medication frequency and drug duration) make up 16% of fatal medication errors.
Prescribing the Wrong Dosage
This medication error happens when your healthcare provider prescribes you the incorrect dosage or amount of a drug. If your body measurements (i.e height and weight) don’t correspond with the prescribed dosage, an overdose may occur or not enough medication is assigned to fully treat your condition – both of which can result in harmful injuries.
While an incorrect dosage may not seem like a serious issue if your condition is minor, it could be life-threatening, regardless of the severity of your condition.
This type of medication error can also happen when pharmacists give you the wrong dosage of a drug, as opposed to your doctor prescribing the wrong dosage. When your pharmacist dispenses a dose that is greater than or less than the amount ordered by the physician, a medication error occurs.
In some cases, your doctor or pharmacist may have written a wrong number or misplaced a decimal point when issuing a prescription (i.e. prescribing 200 milligrams when the correct dosage is 20 milligrams). If doctors fail to write the prescription clearly and neatly, a pharmacist may misinterpret the dosage when dispensing it to the patient.
Prescribing the Wrong Medication
This type of medication error occurs when your doctor, nurse, or pharmacist carelessly prescribes you the wrong drug for your medical condition. In some cases, choosing anan inappropriate medicine can not only fail to heal the patient’s condition, but it can also worsen the patient’s original condition or even cause a new injury.
Failure to Account for Other Medical Conditions
Receiving the wrong type or dosage of medication can be extremely harmful if your doctor has also failed to account for any of your pre-existing medical conditions, such as allergies or diabetes.
If you have multiple conditions, different drugs may have conflicting effects on you that can further worsen your health. If your medical history and conditions aren’t properly accounted for, you could suffer from severe injuries and dangerous long-term effects.
More Types of Medication Errors:
- Ineffectively writing the prescription (unreadable handwriting)
- Failure to take a history of the patient’s prescription or recreational drug use
- Inappropriate drug instructions (i.e prescribing the incorrect number of times the patient should take the drug, the wrong frequency, or an incorrect duration)
- Failure to monitor the patient’s response to prescribed treatment
- Wrong manufacturing of the prescribed drug (i.e. wrong strength, incorrect ingredients, misleading packaging)
- Mixing different prescription drugs
- Failure to properly warn the patient of all risks related to the medication (i.e. side effects)
If your doctor, nurse, or pharmacist has committed any of the above medication errors, they may have acted negligently. If you think you have suffered harmful injuries due to a medication error, you should speak to a medical malpractice lawyer to learn more about your options.
How Do Medication Errors Occur?
The most common causes of medication errors are:
- Ineffective communication between your doctors
- Work overload
- Drug names that sound similar, medications that look alike, and/or medical abbreviations
- Doctor’s poor interpretation of risk
- Poor communication between healthcare providers and their patients
- Computerized system errors
- Incorrect precautionary measures due to insufficient knowledge of patient
- Medical equipment malfunction (i.e unsafe amounts of Intravenous Fluids (IV) drips)
- Lack of drug knowledge and proper medical training
Medication Reconciliation
Studies have revealed that an average hospitalized patient is exposed to at least one medication error per day. While not all of these medication errors result in harm, many health organizations have started to use medication reconciliation during the admission, transfer, and discharge of patients to prevent these types of errors.
According to the Institute for Healthcare Improvement, “Medication reconciliation is the process of creating the most accurate list possible of all medications a patient is taking — including drug name, dosage, frequency, and route — and comparing that list against the physician’s admission, transfer, and/or discharge orders, with the goal of providing correct medications to the patient at all transition points within the hospital.”
In other words, medication reconciliation is the formal process for making the most correct and precise list of a patient’s current medications and comparing the list to all of the healthcare provider’s orders, in order to make sure the patient is prescribed the appropriate medications.